First, you absolutely do NOT need a six-pack to be healthy in any real sense of the word.
We have covered the higher end of body fat levels as it relates to metabolic health in Can You Really Be Healthy At Any Size, but are low body fat percentages inherently healthy?
Is a Six-Pack even healthy?
This is an extremely nuanced question and the individual answer to this question will ultimately depend on how shredded of a six-pack, the processes in play to maintain such a physique, and our personal definition of health.
It is actually very possible that some of the people you see on Instagram with insanely chiseled abs are NOT healthy from a hormonal, immune, GI, bone, and/or psycho-social-emotional standpoint at the moment those photos were taken. (Wow. I know shocking!)
In fact, if you take their blood work, some of these individuals may even be told to seek immediate medical attention and IMO the vast majority of humans probably cannot and should not maintain resting shredded eight packs all year long.
Six-packs and iterations of this degree of leanness are more nuanced and wildly individual. In reading this literature, I have honestly become more and more leery of females and six-packs period and I think in general using the picture above to myopically market health is ignorant, irresponsible, and just really messed up!
If we are strictly talking about physiologic health and adapting to training, people probably shouldn’t live indefinitely in a calorie-restricted or low energy availability state.
The starve yourself forever for longevity is an interesting scientific question, but suffice to say this risky strategy has been shown to severely reduce thyroid and anabolic hormones [1] and whether these longevity findings translate from yeast, fruit flies, and mice to primates eating more healthful diets is a hotly debated topic, as are the mechanistic findings of living at a 25% caloric deficit vs. ad-libitum Western eating [2-7].
Thus, for the majority of us normal, non-biohacker people, who don’t want to spend our life intentionally starving ourselves once we are inside metabolically healthy body composition ranges we can likely work to maximize food consumption and performance/output because in reality that is probably the healthiest and most socially sustainable choice one could make [8].*
For both males and females, this looks like an energy availability of around 40-45 kcals per kilogram of fat-free mass [9-13]. Living with an abundance mindset in our current food environment (eating more while staying weight stable) also seems like a really solid play for results, performance, and the ability to recover from training. I would also argue that the recovery diet back to energy balance in a significant body-fat-reduced state is arguably one of the most critical points in a healthy weight loss journey as well [14, 15].
But, what is Energy Availability?
Energy Availability is a fancy research term that means how many calories you need before taking into account exercise, divided by how much fat-free mass (muscle, bone, organs) you have onboard.
For example, if we have a 155-pound female who is 28% body fat eating 1,500 kcals and burning about 250 kcals in exercise per day that would equal an energy availability of just 24.6 kcal/kg of FFM.
Thus, indefinite caloric restriction is not a viable long-term solution for most people and especially those that care about things like performance, fertility, and I dunno…#LYFE.
“In females, many physiological systems are substantially perturbed at an energy availability of <30 kcal/kg FFM/ day.” (My addition - this is probably around <25 kcal/kg FFM/ day for males given we don’t directly turn calories into baby humans and males are evolutionarily far more expendable.) -Mountjoy et al., 2018 [10]
Eventually, in managing expectations for those seeking body composition changes once we have arrived at a place or some iteration of a place that the person desired, it is likely in our best interest to rev the system.
For the 155lb female with an energy availability of 24.6 kcal/kg FFM that we mentioned above, this likely means slowly stair-stepping her way up to 2,500 kcals per day, and very possibly even more given that the average female in Western environments likely burns a lot more calories than most people think at somewhere around ~2,300 to 2,400 calories per day. While the average male because they are ~20% bigger on average and have more FFM is likely burning well over 3,000 calories per day (and these population averages come from data sets that don't include many people who are religiously resistance training and have FFMs that are on the higher end or even outside the bell-curve) [16-19].
Thus, if we are not going to make the starvation forever for longevity bet it is probably in our best interest to stop asking our bodies to make the choice between adaptation and survival.
Survival will generally always win and without enough energy, the body will rightfully turn the lights down [20-30]. To ultimately bring this back to the Gram, living your life in a sustained low-energy, non-adapting state, because social media, sounds pretty terrible and is very probably not healthy, physically or psychologically.
Everything has a cost and the cost here is potentially the smorgasbord of negative health outcomes that comes along for the ride when we are living in a RED-S state (Relative Energy Deficiency in Sport).
The plethora of physiologic and psychologic negatives here are depicted in the figure below, and unfortunately, most people are unaware of the price of living too lean and not eating enough food.
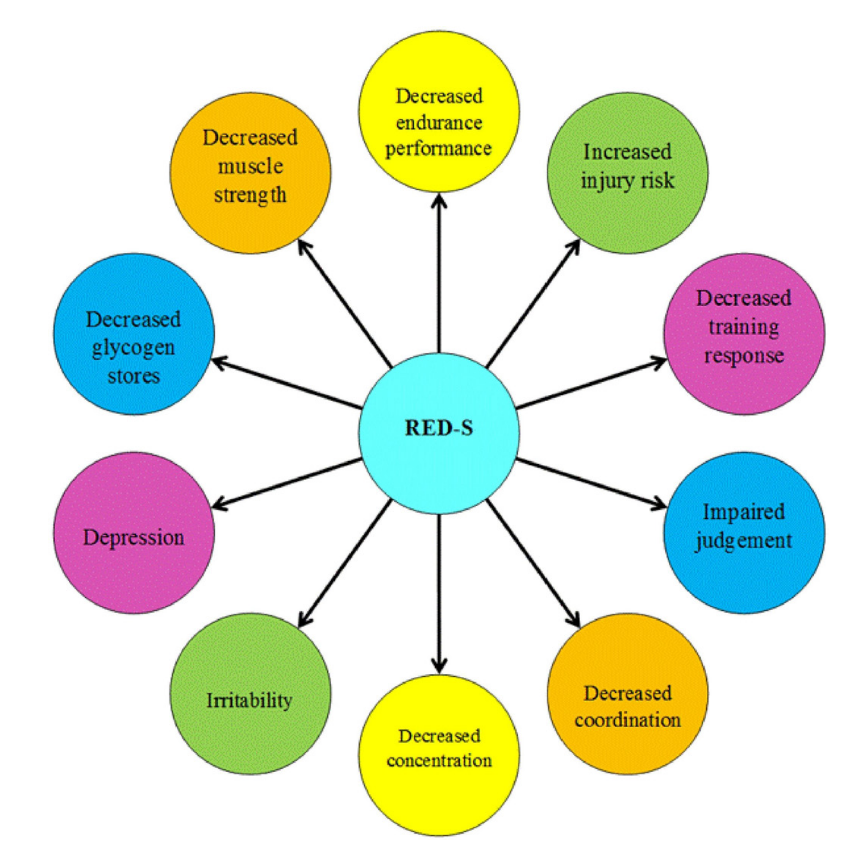
If we are after health, a six-pack is unnecessary, and in many cases, living too lean for most people is likely ill-advised for long-term training adaptations, and in the vast majority of cases, I would vote that we are likely better off flipping the switch to eating MORE, not kind of less forever [31].
Rather than assuming a six-pack is healthy, I think a more interesting and pragmatic question is can a six-pack be healthy?
This is what most aesthetic bros want to know and the answer to this question can absolutely be YES.
Hell, I am not trying to sound holier than though, I like abs and live close to the beach half the year.
Hot Bodies are Hot. They always have been and always will be and that is OK!
Also, there are infinite shades of what people find Hot and I hope that EVERYONE feels sexy AF in their own skin. I am NOT an expert here and most of us in the nutrition and fitness space would likely benefit from reading Come As You Are by Dr. Emily Nagowski and we have talked about some of the deleterious effects of negative Body Image and how to potentially improve it HERE.
After that preamble and under the umbrella that someone in this low body fat and/or low energy availability state is open to change, here is how I would nerdily assess if someone is below their individual low-end body fat percentage. (There are other markers that may be helpful in this scenario, but they are generally expensive and/or high on the subject burden side.)
If you are a female you may want to fill out a LEAF-Q (we don’t have a LEAM-Q yet but I would guess it will likely come out in a few years and maybe sooner [32]). Do you have constant GI symptoms no matter what you eat? Do you feel rested when you wake up in the morning? Also, HERE is the RED-S Clinical Assessment Tool.
From here you can genuinely assess your motivation to train and your results over the last two to three months. Are you excited to train? Do you have nagging injuries that just won’t get better? Have your results improved, stayed the same, or gotten worse with increased effort? See [33-35] for more on NFOR and OTS and [32] for how OTS and RED-S are many times inherently intertwined.
Next, I would likely assess someone’s objective markers of low energy availability that we have talked about previously HERE and HERE.
In males, if Total T3, Free T3, Total Testosterone (SHBG may be High as well), C-peptide, White Blood Cells**, and Triglycerides are all tanked and they are lean or living in a significant body-fat-reduced state I think we can be pretty certain Low Energy Availability is in play.
For cycling females, you would generally have Total T3, Free T3, C-peptide, White Blood Cells, RBCs, Hbg, HCT, Ferritin, Triglycerides, and then menstrual cycle dynamics.*** HOWEVER, this is highly researched in the field of endurance sports and menstrual cycle dynamics (short luteal phase length, anovulation, oligomenorrhea, amenorrhea) are a lot more complex and individually variable than do you have a menstrual flow or not, and “at least 6 months of continuous sampling, in which both ovulation and luteal-phase length are assessed, are necessary to characterize adequately a sedentary, weight-stable woman’s menstrual and ovulatory characteristics.”
Furthermore…
“Serial sampling of blood, saliva, or urine is required to document adequately all of the important ovulatory characteristics (including whether ovulation occurred, as well as luteal-phase adequacy and length) of a single cycle. Continuous longitudinal documentation of hormone levels in large numbers of women is, therefore, virtually impossible to obtain using these sampling techniques…. Another logical question is: why not measure ovulatory characteristics during one cycle and then just monitor cycle intervals over the necessary period of time? Could you not infer that the subsequent cycles, if they are regular and normal in length, are similar in ovulatory status? That would be an accurate strategy if women’s cycles were as stable in ovulatory characteristics as they are in cycle interval. However, ovulatory characteristics are highly variable over time within women.” – Petit and Prior [36] (This is a fantastic book chapter absolutely worth reading).
Whew! Complex.
Honestly, if we are even asking these questions the long-term answer is to probably eat more calories and this is the first step anyways as low energy availability is by far the most likely cause of RED-S [31].
Step One – stair step calories up and reassess. IMO, we also likely want to be straight across, meaning be at our intentional maintenance calories every day of the week, instead of running high-low refeeding schematics. You could also run "maintenance" days plus some higher kcal intake training days as another way to stair-step kcal intake and then if they continue to be weight stable... take the maintenance days up.
By taking this approach you will also inevitably get to know if someone’s current level of leanness is independently leading to dysregulation and this will be very individual and nuanced and likely even relational to their previous body composition [37].
What I can’t give anyone is a realistic time frame for change in this regard. We have seen male bodybuilders come back online when they are sub 10% body fat while consuming an excess of calories and this is somewhat similar to the case study and controlled literature on this population [13, 20, 23, 24, 38].
We have also seen males at 10-20% body fat who have already lost a lot of body fat whose labs and symptomatology mirror stage lean bodybuilders. Whereas, in females Hulmi et al., [22] found that after a three to four-month period of dietary recovery 48% of females still had lab low T3, and De Souza et al., 2021 [21] didn’t see changes to Total T3 until month 12 of increased energy intake in females with menstrual disturbances.
I also don’t think group based lines in the sand like ~20-22% body fat for females and ~10-12% for males are overly helpful here given the likely individual differences, the somewhat massive differences between different body composition assessments, and the fact that many of the body fat estimation equations are not derived from lean populations.
Additionally, many people tend to have the ideology that this is a very small population, but over 45% of recreation exercisers and non-elite endurance athletes may be at risk for low energy availability [31, 39, 40].**** When trying to unravel this potential multi-factorial issue having a medical provider and a psychologist would likely be helpful, but unfortunately many of these professionals have very little exposure to the potential profound and multi-factorial effects of low energy availability states and because of this some individuals have spent tens of thousands of dollars on needless testing when they may have solely needed to take their caloric intake up.
“Much like women with hypothalamic amenorrhea, men with functional hypogonadotropic hypogonadism can recover hypothalamopituitary-gonadal axis function with removal of the energy deficit.” -Dwyer et al., 2019 [37]
What’s ultimately important is the individual, their values and goals, and everything that is going on in their internal and external environment. The objective metrics can be extremely helpful, but we are not our labs or our body composition.
So can a six-pack be healthy?
Physiologically...it depends.
Psychologically...it depends.
To finish this up, I want to quickly review the most popular Body Recomp study to date Longland et al., 2016 [41].
These individuals lost 8.1 to 10.6 lbs of body fat in just four weeks. The higher protein group also gained 2.6 lbs of lean mass. These individuals were at a 40% energy deficit and trained 6 days a week in a supervised setting.
Fantastic results.
AMAZING.
But, now let’s look at the hormonal profile pre and post.
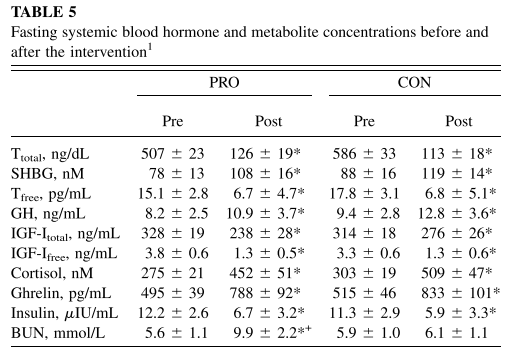
We see that fasting insulin is cut in half, but serum testosterone is now well within the hypogonadal range in the LOW 100s!!!!
SHBG and went up and so did cortisol.
Growth hormone went up, but IGF-1 went down (maybe we have a giggle at the influencers still selling IF and GH boosting), and despite all these hormonal changes individuals gained FFM in the higher protein group (2.4 g/kg) and maintained FFM in the lower protein group (1.2 g/kg)?!?
And here is the thing that tends to surprise everyone these males didn’t go from 14% body fat to 9%.
The PRO group went from ~23% body fat down to ~20% and the Control group went from ~25% down to ~23%.
For context, these subjects on the diet were still consuming ~2,500 to 2,600 kcals per day and the energy prescription of this dietary intervention was 33 kcal/kg of FFM, but this would have likely dropped under 30 kcal/kg FFM because of the number of steps per day and physical activity interventions (doing some rough estimations of caloric expenditure I have it around 26 to 27 kcal/kg FFM when taking into account the PA interventions, but perhaps still over ~25 kcal/kg FFM).
Now I think most of these values (probably including fasting insulin) would normalize back once the training load became habituated and these individuals were brought back up to energy balance at their new body-fat-reduced state (much easier said than done)…but, I don’t know...and that is likely the study and individual interventions we need to be thinking about as we move forward with this question of is weight loss "healthy".
To bring this to females, the Hulmi et al., 2016 [22] bodybuilding study cited above where physique competitors dropped from 23.1% body fat to 12.7% over 20 weeks and 44% lost their menstrual cycle and 74% had lab low T3 at the end of the cut published their metabolic findings in 2019 [42], and the data shows that metabolically these individuals did get “healthier” during that cut.
Now it is hard to extrapolate how clinically meaningful these changes are, but I think these studies do a good job of highlighting the complexity and individual nuance of the question of leanness as it relates to health.
At low levels of body fat with or without low energy availability, we are likely balancing hormonal health (and for many psycho-social-emotional, immune, bone, and GI health) vs. metabolic health markers.
I also think that we will never have concrete answers because at the individual level this kind turns into long-term outcome 4D Chess.
For example, if someone’s rigidity around their diet and body composition decreases their high-sensitivity C-reactive protein (hsCRP) to ZERO would that be better than say an hsCRP of 0.5 mg/L with dietary flexibility, retention of muscle mass, and social embeddedness?
I would probably bet on the latter for both healthspan and lifespan, but I could honestly be wrong…and I can live with that.
So is weight loss healthy if someone is already healthy?
It really does depend…on our values and ultimately what health really means to us.
As a final note, we don't have to add morality to this issue. It is 100% OK if someone wants to get SHREDZ and that aligns with their values and they have informed consent and know the risks. If they know the long-term downsides and want to live that way...also, no problem...just don't use those images and that narrative to myopically market me "health" products. Thanks.
*This entire conversation is predicated on someone being interested in discussing body composition, metabolic health, and longevity, etc., etc.
**If this low energy availability state has been going on for a long time red blood cells, hemoglobin, and/or hematocrit could be low too. They may even be anemic.
***One could add a bone mineral density scan to this list and I think this is a good measurement for most females to have as they age. Lifting males are very likely going to be fine, but high-volume male endurance athletes may want to add this metric in as well.
***These percentages are based on questionnaire and self-reported dietary data, so it is hard to say how under-reporting of energy intake might potentially affect the prevalence on the group level.
REFERENCES:
1. Cangemi, R., et al., Long-term effects of calorie restriction on serum sex-hormone concentrations in men. Aging Cell, 2010. 9(2): p. 236-42.
2. Pifferi, F. and F. Aujard, Caloric restriction, longevity and aging: Recent contributions from human and non-human primate studies. Prog Neuropsychopharmacol Biol Psychiatry, 2019. 95: p. 109702.
3. Mattison, J.A., et al., Caloric restriction improves health and survival of rhesus monkeys. Nat Commun, 2017. 8: p. 14063.
4. Kraus, W.E., et al., 2 years of calorie restriction and cardiometabolic risk (CALERIE): exploratory outcomes of a multicentre, phase 2, randomised controlled trial. Lancet Diabetes Endocrinol, 2019. 7(9): p. 673-683.
5. Maxmen, A., Calorie restriction falters in the long run. Nature, 2012. 488(7413): p. 569.
6. Harper, J.M., C.W. Leathers, and S.N. Austad, Does caloric restriction extend life in wild mice? Aging Cell, 2006. 5(6): p. 441-9.
7. Swindell, W.R., Dietary restriction in rats and mice: a meta-analysis and review of the evidence for genotype-dependent effects on lifespan. Ageing Res Rev, 2012. 11(2): p. 254-70.
8. Aronne, L.J., et al., Describing the Weight-Reduced State: Physiology, Behavior, and Interventions. Obesity (Silver Spring), 2021. 29 Suppl 1: p. S9-S24.
9. Melin, A.K., et al., Energy Availability in Athletics: Health, Performance, and Physique. Int J Sport Nutr Exerc Metab, 2019. 29(2): p. 152-164.
10. Mountjoy, M., et al., IOC consensus statement on relative energy deficiency in sport (RED-S): 2018 update. Br J Sports Med, 2018. 52(11): p. 687-697.
11. Mountjoy, M.L., et al., Relative Energy Deficiency in Sport: The Tip of an Iceberg. Int J Sport Nutr Exerc Metab, 2018. 28(4): p. 313-315.
12. Fagerberg, P., Negative Consequences of Low Energy Availability in Natural Male Bodybuilding: A Review. Int J Sport Nutr Exerc Metab, 2018. 28(4): p. 385-402.
13. Ackerman, K.E., et al., Low energy availability surrogates correlate with health and performance consequences of Relative Energy Deficiency in Sport. Br J Sports Med, 2018.
14. Martins, C., et al., Revisiting the Compensatory Theory as an explanatory model for relapse in obesity management. Am J Clin Nutr, 2020. 112(5): p. 1170-1179.
15. Martins, C., et al., Metabolic adaptation is not a major barrier to weight-loss maintenance. Am J Clin Nutr, 2020. 112(3): p. 558-565.
16. Pontzer, H., et al., Hunter-gatherer energetics and human obesity. PLoS One, 2012. 7(7): p. e40503.
17. Pontzer, H., et al., Daily energy expenditure through the human life course. Science, 2021. 373(6556): p. 808-812.
18. Boushey, C.J., et al., Reported Energy Intake Accuracy Compared to Doubly Labeled Water and Usability of the Mobile Food Record among Community Dwelling Adults. Nutrients, 2017. 9(3).
19. Lichtman, S.W., et al., Discrepancy between self-reported and actual caloric intake and exercise in obese subjects. N Engl J Med, 1992. 327(27): p. 1893-8.
20. Pardue, A., E.T. Trexler, and L.K. Sprod, Case Study: Unfavorable But Transient Physiological Changes During Contest Preparation in a Drug-Free Male Bodybuilder. Int J Sport Nutr Exerc Metab, 2017. 27(6): p. 550-559.
21. De Souza, M.J., et al., Randomised controlled trial of the effects of increased energy intake on menstrual recovery in exercising women with menstrual disturbances: the 'REFUEL' study. Hum Reprod, 2021. 36(8): p. 2285-2297.
22. Hulmi, J.J., et al., The Effects of Intensive Weight Reduction on Body Composition and Serum Hormones in Female Fitness Competitors. Front Physiol, 2016. 7: p. 689.
23. Schoenfeld, B.J., et al., Alterations in Body Composition, Resting Metabolic Rate, Muscular Strength, and Eating Behavior in Response to Natural Bodybuilding Competition Preparation: A Case Study. J Strength Cond Res, 2020. 34(11): p. 3124-3138.
24. Longstrom, J.M., et al., Physiological, Psychological and Performance-Related Changes Following Physique Competition: A Case-Series.J Funct Morphol Kinesiol, 2020. 5(2).
25. Loucks, A.B. and R. Callister, Induction and prevention of low-T3 syndrome in exercising women. Am J Physiol, 1993. 264(5 Pt 2): p. R924-30.
26. Loucks, A.B. and E.M. Heath, Induction of low-T3 syndrome in exercising women occurs at a threshold of energy availability. Am J Physiol, 1994. 266(3 Pt 2): p. R817-23.
27. Loucks, A.B. and J.R. Thuma, Luteinizing hormone pulsatility is disrupted at a threshold of energy availability in regularly menstruating women. J Clin Endocrinol Metab, 2003. 88(1): p. 297-311.
28. Elliott-Sale, K.J., et al., Endocrine Effects of Relative Energy Deficiency in Sport. Int J Sport Nutr Exerc Metab, 2018. 28(4): p. 335-349.
29. Heikura, I.A., et al., Low Energy Availability Is Difficult to Assess but Outcomes Have Large Impact on Bone Injury Rates in Elite Distance Athletes. Int J Sport Nutr Exerc Metab, 2018. 28(4): p. 403-411.
30. Skolnick, A., et al., The Endocrinopathies of Male Anorexia Nervosa: Case Series. AACE Clin Case Rep, 2016. 2(4): p. e351-e357.
31. Dipla, K., et al., Relative energy deficiency in sports (RED-S): elucidation of endocrine changes affecting the health of males and females. Hormones (Athens), 2020.
32. Stellingwerff, T., et al., Overtraining Syndrome (OTS) and Relative Energy Deficiency in Sport (RED-S): Shared Pathways, Symptoms and Complexities.Sports Med, 2021. 51(11): p. 2251-2280.
33. Cadegiani, F.A., et al., Diagnosis of Overtraining Syndrome: Results of the Endocrine and Metabolic Responses on Overtraining Syndrome Study: EROS-DIAGNOSIS. J Sports Med (Hindawi Publ Corp), 2020. 2020: p. 3937819.
34. Grandou, C., et al., Overtraining in Resistance Exercise: An Exploratory Systematic Review and Methodological Appraisal of the Literature.Sports Med, 2020. 50(4): p. 815-828.
35. Kreher, J.B., Diagnosis and prevention of overtraining syndrome: an opinion on education strategies. Open Access J Sports Med, 2016. 7: p. 115-22.
36. Constantini, N.W. and A.C. Hackney, Endocrinology of physical activity and sport. 2nd ed. Contemporary endocrinology. 2013, New York: Humana Press. xi, 558 p.
37. Dwyer, A.A., et al., Functional Hypogonadotropic Hypogonadism in Men: Underlying Neuroendocrine Mechanisms and Natural History. J Clin Endocrinol Metab, 2019. 104(8): p. 3403-3414.
38. Pasiakos, S.M., et al., Effects of testosterone supplementation on body composition and lower-body muscle function during severe exercise- and diet-induced energy deficit: A proof-of-concept, single centre, randomised, double-blind, controlled trial. EBioMedicine, 2019. 46: p. 411-422.
39. Slater, J., et al., Female Recreational Exercisers at Risk for Low Energy Availability. Int J Sport Nutr Exerc Metab, 2016. 26(5): p. 421-427.
40. Lane, A.R., et al., Prevalence of Low Energy Availability in Competitively Trained Male Endurance Athletes. Medicina (Kaunas), 2019. 55(10).
41. Longland, T.M., et al., Higher compared with lower dietary protein during an energy deficit combined with intense exercise promotes greater lean mass gain and fat mass loss: a randomized trial. Am J Clin Nutr, 2016. 103(3): p. 738-46.
42. Sarin, H.V., et al., Substantial fat mass loss reduces low-grade inflammation and induces positive alteration in cardiometabolic factors in normal-weight individuals. Sci Rep, 2019. 9(1): p. 3450.




Related Content
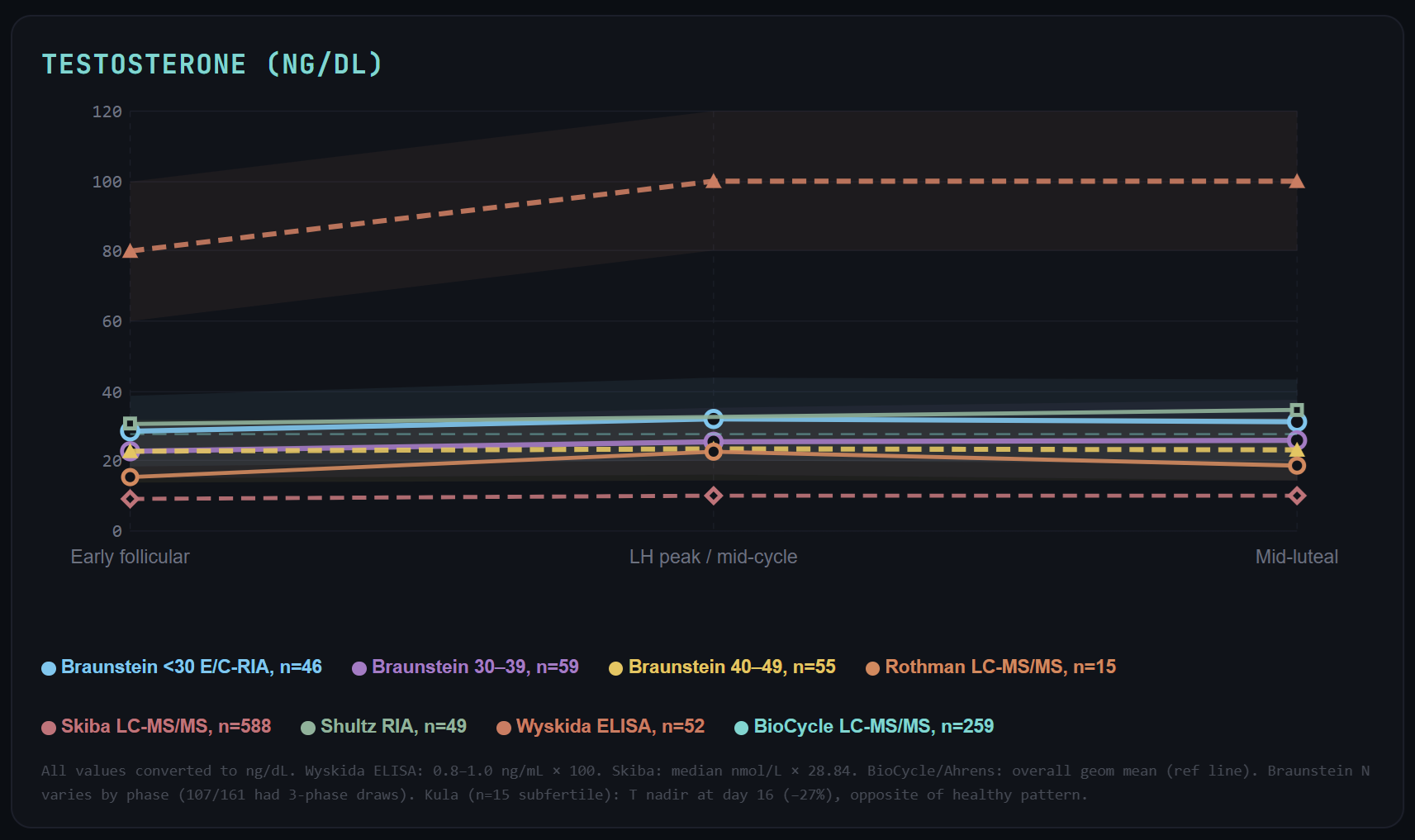
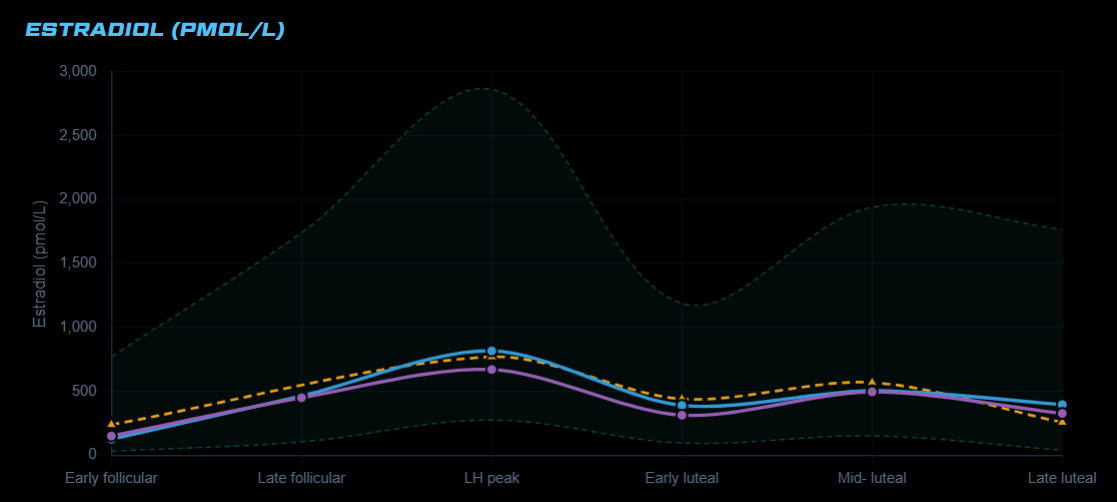
What Are Normal Testosterone, DHT, DHEA-S, and SHBG Levels Across The Menstrual Cycle?
Apr 30, 2026
What Would It Take To Really Map Out The Androgen Signaling Network?
Jan 23, 2026
New Thoughts On Goal Setting and Behavior Change
Jan 02, 2026